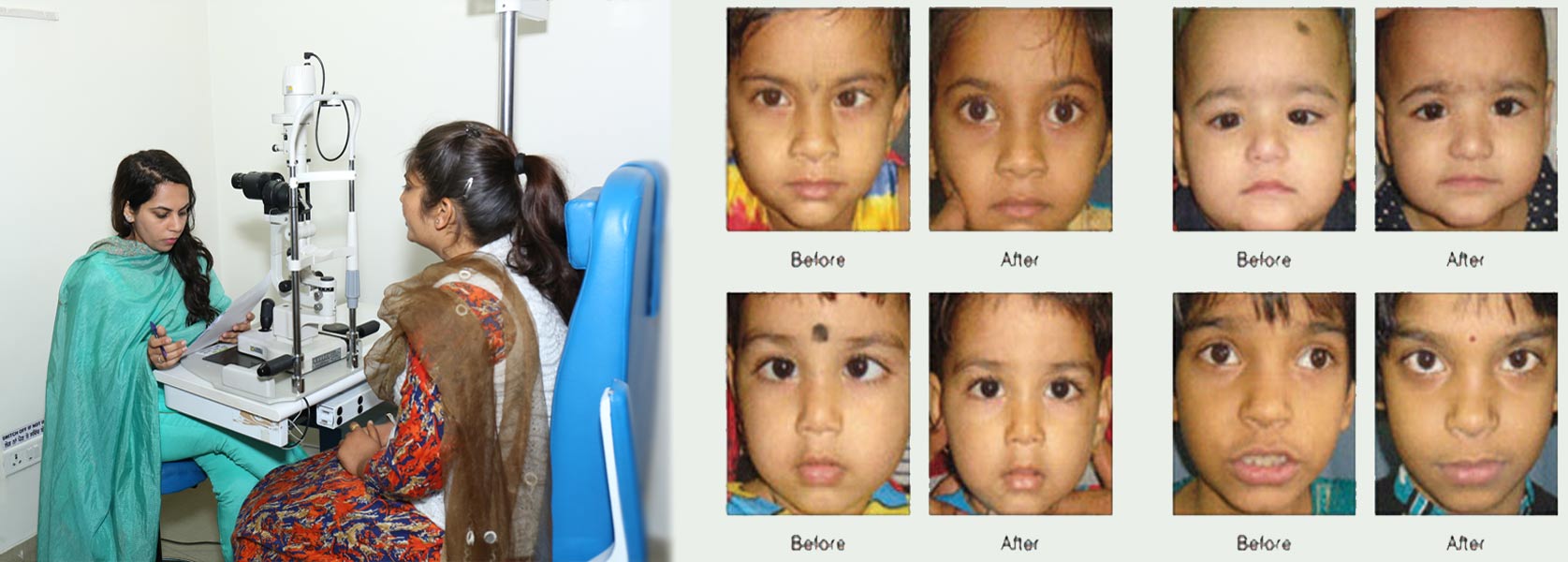
Squint Services
STRABISMUS/SQUINT is a condition that causes an adult or child’s eyes to point in different directions. When looking at an object, a normal person has both eyes pointed straight at that object. If only one eye is looking straight and the other eye is turned away, then that person has strabismus, more commonly known as a squint.
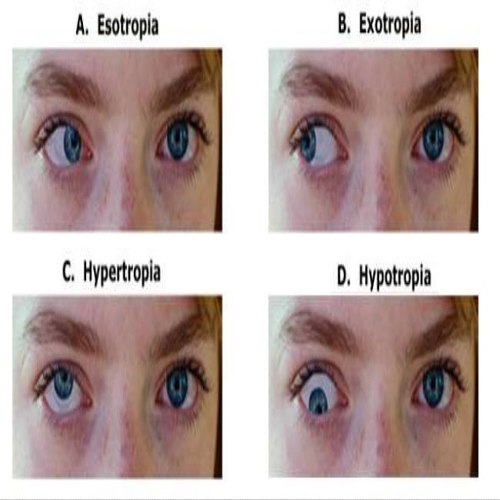
WHAT ARE TYPES OF SQUINTS ?
There are a number of different types of squint in each of these three groups, which have their own individual characteristics and treatments.
1. ESOTROPIAS
An esotropia is the medical name for a convergent squint where one eye turns in towards the nose.
2. EXOTROPIAS
An
exotropia is the medical name for a divergent squint where the one eye turns
outwards.
3. HYPERTROPIAS AND HYPOTROPIAS
These
terms refer to vertical squints where one eye is higher (hypertropia) or lower
(hypotropia) than the fellow eye.
4. PARALYTIC SQUINTS
There are three nerves which send signals to the six eye muscles, these are the third, fourth and sixth cranial nerves. Damage to these nerves as result of poor blood supply to the nerve, pressure on the nerve or head injuries will cause limited eye movements and a squint.
How does a squint affect my child ?
An eye with a squint may become unable to see clearly. This weak eye is called a lazy eye. Lazy eye can only be cured if detected and treated early. The earlier the treatment, the better the results.
A person with a squint can only use one eye at a time. A person with two good eyes will be able to judge distances and depth more accurately than one with a squint. This may affect the choice of your child’s future career and sports. A squint may also affect the appearance and self-confidence of your child. Hence it is sometimes desirable to operate on the child’s squint at an early age. Last, but not least, an eye with a squint may have other conditions which need treatment.
For all these reasons, any infant or child with a squint should be examined by an eye specialist.
WHAT CAUSES A SQUINT ?
There are many causes. It may be due to a disorder of a part of the brain controlling eye movements or it may be caused by weak eye muscles, heredity, cataract and nerve conditions. Also, any eye with poor sight tends to squint.
HOW IS A SQUINT TREATED ?

A child with a squint needs a full eye checkup. This may take time as young children are often uncooperative and may need to be sedated. Even then it may still be necessary to come back another day to confirm the findings or even to put the child to sleep under general anaesthesia to allow an accurate examination.
Treatment may include a combination of patching, eye glasses, eye drops, eye exercises, and surgery. Treatment using the spectacles to correct any refractive errors may cure some types of squint, but to be effective the spectacles must be worn most of the time. As children often resist, the responsibility falls to the parents to make sure they wear their spectacles constantly.
Any lazy eye must be treated. The most effective method is to cover the good eye with a patch so that the child is forced to use the lazy eye. Adequate treatment of lazy eye improves the results of surgery.
Lastly, the eyes must be straightened to improve the appearance and to allow the child to use both eyes together, done usually by surgery. Surgery is only recommended if patching or eye glasses do not work.
How does squint surgery work ?
Squint surgery is an operation on the muscles that move the eye.
Strabismus surgery involves tightening the weak muscles and/or loosening the stronger ones so that the eyes are positioned better. Special absorbable stitches will hold the eye muscles in their new position.The surgeon will not cut the skin around the eye, take the eye out of its socket or use any lasers during the operation.
Sometimes both eyes need to be operated upon but this provides hardly any risk to the eye.
- Eye muscle surgeries typically correct strabismus and include the following:
- A. Loosening / weakening procedures
- Recession involves moving the insertion of a muscle posteriorly towards its origin.
- Myectomy
- Myotomy
- Tenectomy
- Tenotomy
- B. Tightening / strengtheningprocedures
- Resection involves detaching one of the eye muscles, removing a portion of the muscle from the distal end of the muscle and reattaching the muscle to the eye.
- Tucking
- Advancement is the movement of an eye muscle from its original place of attachment on the eyeball to a more forward position.
- C. Transposition / repositioning
procedures
- Adjustable suture surgery is a method of reattaching an extraocular muscle by means of a stitch that can be shortened or lengthened within the first post-operative day, to obtain better ocular alignment.
Strabismus surgery is a
one-day procedure. The patient spends only a few hours in the hospital with
minimal preoperative preparation. The average duration of the surgery is
variable. After surgery, the patient should expect soreness and redness. In
cases of re-operations, more pain is expected. Resection of the muscles is more
painful in the post operative period than recession. It also leaves redness
that lasts longer and may cause some vomiting in the early post operative
period.
The surgeon will provide the patient with a cover for his or her eyes that prevents light from entering. It is advisable for the patient to wear this, since stimulus to the eye (e.g., light, rolling of eyes) will cause discomfort.
Will the operation be successful?
Almost operations will show an improvement in their appearance. Some will be able to use both eyes together and improve their judgement of depth and distances. The degree of success depends on factors such as the type and size of the squint and the presence of good vision in both eyes. In complicated cases, further operations may be necessary.
What are the risks of surgery ?
This is a minor operation. As such, life-threatening or blinding complications are very rare. Children will be put to sleep under general anaesthesia, but this is very safe if your child is healthy. Sometimes double vision may occur after the operation, but this usually recovers without treatment after a few months.
How long will my child take to get well?
Your child’s surgery will usually be performed as a day surgery. He will be admitted in the morning and will be allowed home on the same day after the operation. After discharge from the hospital, the next appointment will usually be on the next day and again within one week. There is little or no pain after the operation and the eye is not patched, allowing the child to go back to normal study and play after a few days. Swimming should be avoided for a month.
Does it run in the family?
Most people with squints do not have affected relatives and are of normal intelligence. However, since it occasionally runs in families, it is wise to check the rest of your children if a family member has a squint.
Summary
A squint is a common condition affecting young children that may affect their sight, appearance and confidence it not detected and treated early. Every young child should have his eyes checked regularly. The treatment of squint is safe and effective but needs the full cooperation of parents.
AMBLYOPIA

Amblyopia, also called lazy eye, is a disorder of sight due to the eye and brain not working well together. It results in decreased vision in an eye that otherwise typically appears normal. It is the most common cause of decreased vision in a single eye among children and younger adults
The cause of amblyopia can be any condition that interferes with focusing during early childhood. This can occur from poor alignment of the eyes, an eye being irregularly shaped such that focusing is difficult, one eye being more nearsighted or farsighted than the other or clouding of the lens of an eye. After the underlying cause is fixed, vision is not restored right away, as the mechanism also involves the brain. Amblyopia can be difficult to detect, so vision testing is recommended for all children around the ages of four to five.
Early detection improves treatment success. Glasses may be all the treatment needed for some children. If this is not sufficient, treatments which force the child to use the weaker eye are used. This is done by either using a patch or putting atropine in the stronger eye. Without treatment, amblyopia typically persists into adulthood. Evidence regarding treatments for adults is poor.
Amblyopia begins by the age of five. In adults, the disorder is estimated to affect 1–5% of the population. While treatment improves vision, it does not typically restore it to normal in the affected eye. Amblyopia was first described in the 1600’s. The condition may make people ineligible to be pilots or police officers. The word amblyopia is from Greek ἀμβλύς amblys meaning “blunt” and ὤψ ōps meaning “sight”.
Signs and symptoms
Many people with amblyopia, especially those who only have a mild form, are not aware they have the condition until tested at older ages, since the vision in their stronger eye is normal. People typically have poor stereo vision, however, since it requires both eyes. Those with amblyopia further may have, on the affected eye, poor pattern recognition, poor visual acuity, and low sensitivity to contrast and motion.
Amblyopia is characterized by several functional abnormalities in spatial vision, including reductions in visual acuity, contrast sensitivity function, and vernier acuity, as well as spatial distortion, abnormal spatial interactions, and impaired contour detection. In addition, individuals with amblyopia suffer from binocular abnormalities such as impaired stereoacuity (stereoscopic acuity) and abnormal binocular summation. Also, a crowding phenomenon is present. These deficits are usually specific to the amblyopic eye. However, subclinical deficits of the “better” eye have also been demonstrated.
People with amblyopia also have problems of binocular vision such as limited stereoscopic depth perception and usually have difficulty seeing the three-dimensional images in hidden stereoscopic displays such as autostereograms. Perception of depth, however, from monocular cues such as size, perspective, and motion parallax remains normal.
Types
- Amblyopia has three main causes:
- Strabismic: by strabismus (misaligned eyes)
- Refractive: by anisometropia (difference of a certain degree of nearsightedness, farsightedness, or astigmatism), or by significant amount of equal refractive error in both eyes
- Deprivational: by deprivation of vision early in life by vision-obstructing disorders such as congenital cataract
Diagnosis
Amblyopia is diagnosed by identifying low visual acuity in one or both eyes, out of proportion to the structural abnormality of the eye and excluding other visual disorders as causes for the lowered visual acuity. It can be defined as an interocular difference of two lines or more in acuity (e.g. on Snellen chart) when the eye optics is maximally corrected. In young children, visual acuity is difficult to measure and can be estimated by observing the reactions of the patient reacts when one eye is covered, including observing the patient’s ability to follow objects with one eye.
Stereotests like the Lang stereotest are not reliable exclusion tests for amblyopia. A person who passes the Lang stereotest test is unlikely to have strabismic amblyopia, but could nonetheless have refractive or deprivational amblyopia.It has been suggested that binocular retinal birefringence scanning may be able to identify, already in very young children, amblyopia that is associated with strabismus, microstrabismus, or reduced fixation accuracy. Diagnosis and treatment of amblyopia as early as possible is necessary to keep the vision loss to a minimum.
Screening for amblyopia is recommended in all people between three and five years of age.
Treatment
Treatment of strabismic or anisometropic amblyopia consists of correcting the optical deficit (wearing the necessary spectacle prescription) and often forcing use of the amblyopic eye, by patching the good eye, or instilling topical atropine in the good eye, or both.
Concerning patching versus atropine, a drawback is seen in using atropine; the drops can have a side effect of creating nodules in the eye which a correctional ointment can counteract. One should also be wary of overpatching or overpenalizing the good eye when treating amblyopia, as this can create so-called “reverse amblyopia”. Eye patching is usually done on a part-time schedule of about 4–6 hours a day. Treatment is continued as long as vision improves. It is not worthwhile continuing to patch for more than 6 months if no improvement continues. Treatment of individuals age 9 through to adulthood is possible through applied perceptual learning.
Deprivation amblyopia is treated by removing the opacity as soon as possible followed by patching or penalizing the good eye to encourage the use of the amblyopic eye. The earlier the treatment is initiated, the easier and faster the treatment is and the less psychologically damaging. Also, the chance of achieving 20/20 vision is greater if treatment is initiated early.
One of the German public health insurance providers, Barmer, has changed its policy to cover, as of 1 April 2014, the costs for an app for amblyopic children whose condition has so far not improved through patching. The app offers dedicated eye exercises which the patient performs while wearing an eyepatch.